Table Of Contents
- History
- Benefits
- Surgery Day
- Recovery
- Diet
- Vitamins & Supplements
- Complications
- Can it be Stretched?
- Expected Weight Loss
- Emotional & Mindset Changes
- Tools For Success
Gastric sleeve surgery, also known as the sleeve gastrectomy, has become a popular choice for patients seeking excellent weight loss in a straightforward procedure that doesn’t require the maintenance and long-term complication rates of a Lap Band.
History
On January 1st, 2010 United Healthcare added gastric sleeve surgery to their list of covered surgeries for weight loss. Over the following two years, almost every other major insurance company followed suit. From 2010 to the 2018 gastric sleeve surgery became the fastest growing bariatric surgery procedure in the United States (estimated growth rates from BOLD/MBSAQIP).
Why?
It’s very difficult to get insurance companies to approve new procedures. So why would they approve gastric sleeve surgery?
- The evidence showed significant weight loss with low complication rates.
- Surgeons were already performing the procedure and insurance was paying!
Number 2 deserves some explanation.
Super Obese individuals (people with a Body Mass Index over 45) have an increased risk during any surgery. And the longer the time under anesthesia, the greater the risk. Gastric bypass surgery can last over 2 hours. Duodenal switch surgery often takes over 4 hours. That’s a long time to be under anesthesia.
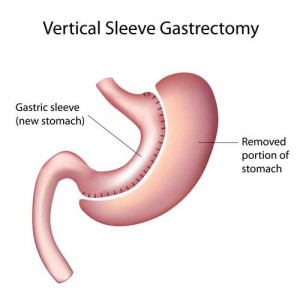
So surgeons started breaking the procedure up into two stages. The first stage was to reduce the size of the stomach. The second stage would be done a year later after the patient lost some weight. The second stage of the procedure would include bypassing some of the intestines to reduce calorie absorption.
So surgeons started coding the first part of the procedure as the first half of a duodenal switch. Insurance was paying.
When patients came back a year later, they had lost so much weight that a second procedure wasn’t necessary.
Studies like this one started to emerge (Randomized clinical trial of laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy for the management of patients with BMI < 50 kg/m2). Complication rates were low and weight loss was as good, if not better, than gastric bypass. And because the surgery took less time and was less complicated to perform, surgeons liked it.
Patient Feedback
Patients also liked the procedure. After surgery and often for months after the procedure patients noticed they weren’t hungry. Some patients had to remind themselves to eat.
Soon patients were asking their doctors about gastric sleeve surgery.
Later, research showed that the hunger producing hormone ghrelin was significantly lowered in gastric sleeve patients. It’s believed that the area of the stomach removed during gastric sleeve surgery produces much of the hormone ghrelin. While gastric bypass patients experienced less hunger, it seemed to be more pronounced in gastric sleeve patients.
Potential Benefits to Patients
Gastric sleeve surgery has the benefits below:
- May reduce hunger.
- The hunger inducing hormone ghrelin is reduced by removing a portion of the stomach largely responsible for its production.
- Reduction of hunger occurs in most patients but not all.
- Shorter operating time compared to gastric bypass.
- Does not re-route intestines.
- No dumping syndrome.
- While dumping syndrome can be a tool to reinforce good eating habits, it’s very unpleasant.
- The pylorus remains intact and sugars have time to digest since the intestines remain untouched.
- No adjustments are needed. The Lap Band requires regular adjustments (doctor visits).
- No foreign objects are left in the body. The Lap Band leaves a silicone band around the upper portion of your stomach.
- Weight loss occurs over 18 months.
- Gastric bypass weight loss is very quick. The majority of weight loss occurs in the first year.
- Lap Band is gradual and requires major lifestyle changes for success. The majority of weight loss occurs over 3 years.
Why Your Surgeon Prefers Sleeve Gastrectomy Over Lap Bands

Guess what? Your surgeon may prefer gastric sleeve or bypass over Lap Bands. Surgeons want you to be successful. Most surgeons care about getting you healthy. But, they also know that you’re a future referral source. You are a future success story.
If your surgeon has been performing bariatric surgery for long enough he or she has seen patients that lose little or no weight with a Lap Band.
This doesn’t mean the band isn’t working. It just means that certain patients cannot implement the lifestyle changes (3 small meals a day, high protein, exercise, low carbs, etc.) that are needed to be a success with the Lap Band.
The failure to lose weight is significantly less with gastric bypass or gastric sleeve surgery. Granted, after the weight comes off, it’s up to the patient to keep it off.
For a surgeon that is trying to help, it’s difficult to identify patients that are truly dedicated to implementing exercise and healthy, nutrient dense foods into their diet.
It’s a much better bet and ‘safer’ to recommend bypass or sleeve.
Surgery Day
 So you want to know what to expect on the day of surgery? Expect to be scared, nervous, and expect everything to go well.
So you want to know what to expect on the day of surgery? Expect to be scared, nervous, and expect everything to go well.
Again, gastric sleeve surgery is a very straightforward procedure with low complication rates. When serious complications do happen, they usually occur the first few days after surgery. So rest easy for your procedure.
You’ll likely be scheduled for an early morning surgery. However, this depends on the surgeon’s and hospital’s schedule.
Prior to surgery you will have followed your two week pre-op diet. You should know what to bring to the hospital. And you’ll know that you can’t eat anything after midnight the night before. Don’t cheat! Surgeries get cancelled all the time because people eat or drink prior to surgery. And if you vomit during your procedure you can get pulmonary aspiration. This is when the contents of your stomach regurgitate and get stuck in your airways. This can be fatal or cause aspiration pneumonia.
Don’t chew gum, drink water, chew tobacco, or take any medications not approved by your surgeon. These may cause your surgery to be cancelled.
You’ll check into pre-op and meet your nurse and your Anesthesiologist. You’ll change into your hospital gown, removing any jewelry, watches, etc.. You’ll then sign the needed consents and get an IV. You’ll be given medication to help you relax. Your circulating nurse (the nurse that will be with you in the OR) will come meet you and wheel you back to the OR. Then you’ll be asked to breath in from a face mask and count backwards.
When you wake up you’ll be in recovery and your family will be invited in shortly thereafter. Once cleared, you’ll be wheeled up to your room where the TV and your pain pump will be your new best friend for the night.
Typically, within the first 5 hours after surgery, you’ll be asked to get up and take a few steps. This helps reduce the risk of blood clots and help alleviate some of the shoulder pain associated with the CO2 left in your abdomen from the surgery.
Recovery
Recovery from gastric sleeve surgery is painful for some and ‘not too bad’ for others. Each person experiences pain differently and different pain medications work better than others for different individuals.
Some sleeve procedures are outpatient (you can leave the same day as your procedure) and many require 1 or 2 days in the hospital to recover. Some surgeons prefer 3 days while others are comfortable letting you leave the day after surgery.
As always, it’s important that you follow the doctors orders.
Below are some general guidelines after you are discharged from the hospital. You should have more specific guidelines to follow in your discharge instructions or post-op manual.
- Sip your liquids constantly.
- It’s easy to become dehydrated. You aren’t getting any liquids from food your first week post-op. Sip slowly, but makes sure you drink plenty.
- Bowel movements
- Bowel movements may be difficult or painful. This is normal.
- However, don’t hesitate to call your surgeon if you are having issues.
- Constipation is normal the first week post-operative. Your pain medications can increase constipation.
- Medications
- Don’t be a tough guy. Take your pain medication when you need them.
- You may receive a prescription for Protonix to decrease the acidity in your stomach. This helps with heartburn and may reduce pressure on your healing pouch.
- Unless otherwise advised by your surgeon, you can resume taking your medications. All non-time-released medications will likely need to be crushed. Any medication that is time-released should be switched, if possible, to non-time released. Do not crush time-released medications. Ask your doctor about your diabetes medication.
- Activity
- Walk, walk, walk.
- Walk as much as you can. This helps the healing process and starts you on the path to include exercise daily.
- Don’t lift anything heavy. This can put undue pressure on your stitches and torso which will be sore.
- You will feel fatigued and tired for up to a month after surgery.
- This is due to the reduced calorie consumption. Your body is adjusting.
- Walk, walk, walk.
- Showering & Bathing
- Don’t bathe or sit in a hot tub for the first 3 weeks after surgery.
- Showering is typically OK.
- Going back to work.
- You can typically return in 2 to 4 weeks depending on the physicality of your job.
- Most people return after 4 to 6 weeks at full strength.
 When to call the ER?
When to call the ER?
- Fever over 101.5 with shaking or the chills.
- Pain that increases over time.
- Redness, warmth or pus draining from incision sites.
- Persistent nausea.
- Inability to swallow liquids.
Remember, don’t hesitate to call your surgeons office if you are worried that something is wrong. You’re not bothering them.
This article walks you through the details of recovery from gastric sleeve surgery.
Pre and Post-Op Diet
Your diet is going to change after gastric sleeve surgery.
In fact, your diet has to change 2 weeks prior to surgery. So if you’re planning on having a ‘last meal,’ you’ll want to do it before you start the pre-op diet.
Pre-Op Diet
Your pre-op diet will start 2 weeks before your surgery date. The pre-op diet is important because it helps to reduce the size of your liver prior to surgery. This makes surgery easier for your surgeon and reduces your intra-operative risks.
Details on a typical pre-op diet can be found here.
Post-Op Diet
 They say it takes tasting a food 20 times to develop a liking for it. Keep that in mind as you struggle through the first few months of adopting a new diet after surgery. With a small stomach, it’s utterly important that the food you do eat is nutrient dense. This means you should be eating foods like vegetables, lean protein sources and whole grains.
They say it takes tasting a food 20 times to develop a liking for it. Keep that in mind as you struggle through the first few months of adopting a new diet after surgery. With a small stomach, it’s utterly important that the food you do eat is nutrient dense. This means you should be eating foods like vegetables, lean protein sources and whole grains.
Most doctors recommend you eat a good portion of your calories via lean meat. However, it should be noted that there are some very successful vegetarians that have had gastric sleeve surgery.
Dr. Garth Davis at The Davis Clinic in Houston is a bariatric surgeon and a vegetarian. Many of his patients have become vegetarians with great success.
Your post-op diet greatly depends on how far out you are from surgery. The stages below are typical recommendations after gastric sleeve surgery. For a more detailed look what you can and can’t eat after surgery, we recommend this article.
Stage 1 – The first week after surgery
- Clear liquids only. These include:
- Water
- Decaf Tea
- Sugar-free Popsicles
- Broth
Stage 2 – Week 2
- Full liquid diet with protein shakes.
Stage 3 – Week 3
- Soft-pureed foods. These include:
- Soups
- Scrambled Eggs
- Cottage Cheese
Stage 4 – Week 4
- Soft foods.
- Boiled chicken.
- Fish
- Cereal
- Mashed potatoes.
Stage 5 – Week 5 and beyond
- Introducing real foods.
- Introduce small amounts of foods.
- Chew well and eat slowly.
- Eat 3 small meals a day.
- Eat a small, healthy, nutrient dense food as a snack if needed.
- Get your protein but don’t forget vegetables and fruit.
Daily Vitamins & Supplements
You’ll need to ensure you are getting enough vitamins and minerals after gastric sleeve surgery. This is also true for gastric bypass (slightly more supplements are required) and true for adjustable gastric band or balloon patients (less vitamins are required). Below is a list of typical vitamins and protein supplements for a gastric sleeve patient.
Multivitamin with Minerals – Most patients use chewable vitamins right after surgery. Follow the directions from your bariatric doctor’s office. You may need to take one in the morning and one at night (depending on the brand).

Below are a few options for bariatric multivitamins:
- Bariatric Advantage
- BariMelts
Iron – It’s important to talk to your doctor and follow his or her recommendation.
- You need at least 45 mg of iron after sleeve gastrectomy
- Do not take with your Calcium Citrate.
Calcium Citrate – Taken 2-3 times daily, in doses of 600 mg or less.
- Do NOT take calcium at the same time as iron.
- Wait at least 2 hours between taking your multivitamin/iron and your calcium.
- 1200-1500 mg daily.
Vitamin B12 –
- At least 350 mcg per day
Vitamin B1 (Thiamin) –
- At least 12 mg per day
Protein Supplements
Protein is important after gastric sleeve surgery. It’s recommended that you get at least 60 grams of protein per day after surgery. However, most physicians prefer a bariatric specific protein supplement. Below are some common options for bariatric protein supplements.
- Genepro
- Bariatric Advantage
- Nectar
These can be purchased online from bariatric supplement stores, or directly from the Baritastic App if you have that downloaded to your smart phone.
Complications
You should have a good understanding of possible complications during and after your surgery. The most worrisome complication from gastric sleeve surgery is a staple line leak.
Staple line leaks can occur during or after surgery. During surgery, they are typically noticed and fixed before completing the surgery – no big deal. However, if they go unnoticed, you will start to get sick shortly after surgery.
Staple line leaks typically occur during the first month after surgery. They can be triggered by eating improper foods (always follow your post-op diet) or from the tissues of your stomach not healing. This, in turn, leads to the staples detaching from the thin, devascularized tissue which then leads to a leak.
A staple line leak leads to a major infection as your stomach juices enter your abdomen. The signs and symptoms are tachycardia (rapid heartbeat), fever, chest pain, and pain in your belly.
Most staple line leaks occur within 14 days of surgery. See your doctor immediately if any of these symptoms are present.
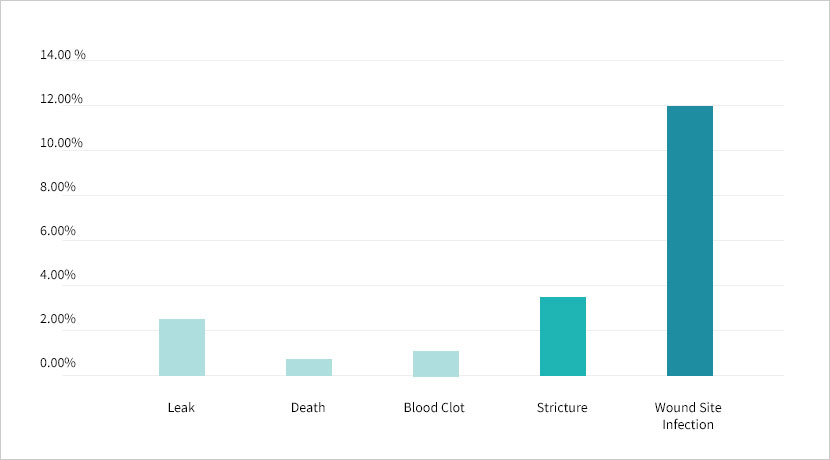
The risk of death from gastric sleeve surgery is low. The chart below shows the risk of the more serious complications with gastric sleeve surgery.
This article is a full list of the most common complications along with their signs and symptoms.
Can it be Stretched?
 You can stretch your stomach after gastric sleeve surgery. The inside of your stomach is lined with rugae. These are folds of tissue that expand and contract in relation to the amount of food that enters your stomach.
You can stretch your stomach after gastric sleeve surgery. The inside of your stomach is lined with rugae. These are folds of tissue that expand and contract in relation to the amount of food that enters your stomach.
When they expand, your stomach sends a signal to your brain that you are full. When they contract, they push the food into your intestines for further processing. Once the stomach is empty, a hormone called ghrelin is released that triggers hunger again.
These signals can get skewed when your stomach is constantly stretched from too much food. This article details how this happens and why it’s important to get back on track quickly after binging.
Below are a few tips to reduce the risk of stretching your stomach.
- Drink water an hour before and an hour after you eat. This gives your body time to digest the food and make room for fluids and vice versa. Don’t eat and drink at the same time.
- Don’t drink carbonated beverages. The carbonation can put unneeded pressure on your stomach.
- Eat small, healthy snacks if you get hungry in-between meals.
- Plan your meals. Focus on small portions of nutrient dense foods. Nutrient dense foods keep you full longer and give you the nutrients that you need.
Remember, if you overeat once, you haven’t ruined your new stomach. Get back on track as quickly as possible.
Expected Weight Loss
On average, gastric sleeve patients will lose about 60% of their excess weight. Excess weight does not mean total weight. If you weigh 300 lbs, you will not weigh 120 lbs after surgery. To calculate your expected weight after surgery, use our calculator.
You should know that you can lose more or less than 60%. There are many examples of people that have implemented exercise (marathons even) into their daily lives and have far exceeded the 60% mark. Some people who revert back to poor eating habits lose less than 60%.
The key to success (exceeding the 60%) is implementing the changes needed to keep the weight off. Below is a list of the mean average excess weight loss 5 years after surgery.
Hitting Weight Plateaus
Gastric sleeve surgery will make you lose weight fast. However, similar to any diet, you’ll hit a wall (plateau) at some point. This means you’ll lose weight, and you’ll lose it fast, and then all of the sudden you’ll stop losing.
When the weight loss stops, often only 6 months after surgery, patients freak out (that’s the technical term).
Why does it happen?
Your body is constantly seeking something called homeostasis. Homeostasis is a process that maintains the human body’s internal environment in response to changes in external conditions.
So when food decreases significantly (external condition), your body adjusts internally to create stability (stable weight). So, to counteract the lack of food in your environment, the body slows down your basal metabolic rate – your metabolism slows down and you hit a wall. You haven’t changed your eating or exercise habits and you hit a wall before you reach your target weight.
How do you get past a plateau?
To get past a weight loss plateau, you need to add a new external change. This is typically done by increasing exercise. But what if you are already spending as much time in the gym as possible? You need to look for other ways. Simply adding a couple of 30 second planks morning and night may be all you need. Can you take an extra walk before bed? Are you taking the stairs at work?
It may be worthwhile to meet with a personal trainer and have them design a workout plan that you can maintain. Their plan should be more intense than your current workout.
You may need to consider adding a small healthy snack in between meals to speed up your metabolism.
Have your bariatric dietitian review your weight loss. Download an app like Baritastic and start tracking all of your food consumption. Share your food logs with your dietitian and ask him/her to review it and look for areas to improve.
Learn more about weight plateaus and how to break them.
Emotional & Mindset Changes
 This topic is often passed over for topics with clinical studies backing them up. However, it’s important to know that emotional changes do happen after surgery. And you should be prepared for them.
This topic is often passed over for topics with clinical studies backing them up. However, it’s important to know that emotional changes do happen after surgery. And you should be prepared for them.
Immediately after surgery, you will start to lose weight very quickly. Drastic weight loss leads to changes in hormone production. Changing levels of estrogen and testosterone results in mood swings. Let your family know that this is probable, particularly in the first 2 months after surgery.
On top of the mood swings, you will be tired. Tired and moody people tend to be less than pleasant. Have faith, this goes away. And not everyone experiences mood swings.
Personality Changes
One other interesting, admittedly anecdotal change is related to personality. ObesityCoverage has a podcast where we interview patients after surgery. About 50% of our interviewees have mentioned that they noticed a change in their personality starting a few months after surgery.
What kind of changes? After weight loss surgery patients tend to be less of a pushover. Is this a result of the required therapy/counseling sessions pre and postoperatively? Is it because of a new self-confidence? Or is it because weight loss surgery requires you to take a hard and honest look at yourself (everything from diet habits, lifestyle habits, and relationships)? It’s probably a mix of all of those.
Regardless of what causes it, all of our interviewees have said the changes are a good thing.
Relationship Changes
If you read enough about weight loss surgery, you’ll notice a fairly high incidence of divorce. There are no clinical studies to back this up, so don’t assume this is going to happen to you. However, you should know that there are many stories of divorce after gastric sleeve surgery.
From interviewing a number of patients (this podcast is about divorce after surgery) who have had weight loss surgery and subsequently found their marriage failing, below are some important takeaways.
- Your partner may become insecure as you start to lose weight and gain self-confidence.
- You may be less tolerant of certain behaviors from your spouse. Excessive drinking, smoking, anger, passive-aggressive behavior, are examples of this.
- You may find that your husband doesn’t share the same desire to eat and live a healthy life. This can be fine if you find friends to help support you.
As a result of your therapy sessions, you may find yourself taking a close look at your friends. The people you surround yourself with should make you a better person and help you reach your health and work goals. This doesn’t mean that you need to get rid of all of your friends. But it does mean you should try to surround yourself with people that want to make you better.
Gastric Sleeve Maintenance
Gastric sleeve surgery doesn’t require regular band fills as the Lap Band does. But it does require maintenance. There are no tune-ups with a gastric sleeve. Once it’s done, it’s done. However, you do have to ensure you are doing the right things to create lasting weight loss.
Diet Maintenance
It’s utterly important that you follow the new dietary guidelines for the rest of your life. Falling back into old habits is easy. You can regain weight after gastric sleeve surgery.
Exercise Maintenance
You must ensure that you continue to exercise at a minimum of 3 times per week. It’s preferable to workout 5 to 7 days a week for 30 minutes. Exercise can be walks, runs, fitness videos, etc. The goal is to get moving and increase your heart rate. In turn, you’ll burn calories.
Mood Maintenance
Maintaining a positive attitude 100% of the time is impossible. Everyone has bad days. For people with food addictions, a state of depression can trigger food cravings. When you’re depressed, food becomes a comfort. Being healthy becomes secondary to finding immediate comfort.
On a daily basis, you should take notice of your mood. Are you motivated? Have you been spending time with friends? Are you abnormally tired?
Losing the battle with food often starts with a sad or angry mood. Ensure you pay attention to your mood and actively manage it by implementing healthy activities to improve your well-being.
While you will have bad days, don’t let those bad days become bad weeks or months. If you have a bad day and seek comfort from food, it’s ok. Tomorrow is a new day. Don’t let overeating become a vicious cycle that leads to a stretched stomach and weight gain.
Tools For Success
There is a lot of information available online. There are apps to track your food, books to help you get and stay healthy. Below is a list of our 5 favorite tools for success.
 Join a Forum
Join a Forum
- It’s important to find friends, ask questions, and stay motivated.
- Join a Facebook Group
- Facebook makes it easy and private to share your success with a real face (profile). There are some very active groups. And you must request to join them.
- Your current friends won’t know you’re part of the group and they won’t see your posts (they’re private).
- My favorite for gastric sleeve surgery is the Baritastic Social group. This group has supportive members and negativity is not allowed.
- Download the Baritastic App
- Track exercise, nutrition, water and more.
- Local Support Groups
- Don’t forget to attend each month.
- Your surgeon will offer these either through the hospital or at his/her clinic. They are invaluable for making friends and staying committed.
- If you can’t find a support group in your area, check the OAC’s list of local support groups here.
- Document your progress in a public place.
- When you let your friends, family, and strangers know that you’ve had or will have bariatric surgery, you add a level of accountability.
- You can do this in a forum, Facebook group, or with your friends and family.
- Feedback on your journey will help you stay motivated and encourage you to become a superstar.
Conclusion
Gastric sleeve surgery is a long journey. On average, it takes close to two years to reach your target weight.
It takes changing an entire lifetime of unhealthy habits to keep the weight off. It’s not the easy way out. It takes dedication, perseverance and daily work (forever). Keep learning, reinforcing good habits, and celebrating your small victories.
The farther you get from surgery, the less you will think of yourself as a sleeve patient and the more you’ll consider yourself someone that chooses to be ‘healthy.’
Remember gastric sleeve surgery is a tool. It helps you lose weight so you can implement the healthy changes that will forever change your life.