Table of Contents:
- History
- Benefits
- Surgery Day
- Recovery
- Diet
- Dumping Syndrome
- Vitamins & Supplements
- Can it be Stretched?
- Expected Weight Loss
- Saggy Skin
- Emotional Changes
- Risks and Downsides
- Books and Tools For Success
- Conclusion
History
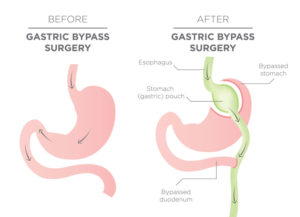 Weight loss surgery was developed using two different approaches. One of these approaches used techniques of restriction that limited the intake of calories while the other focused on techniques of malabsorption that restricted the amount of calories absorbed by the body.
Weight loss surgery was developed using two different approaches. One of these approaches used techniques of restriction that limited the intake of calories while the other focused on techniques of malabsorption that restricted the amount of calories absorbed by the body.
The first of these attempts was the jejuno-ilial bypass by A.J. Kremen in 1954, which concentrated on the latter of the two approaches. However, this surgical procedure resulted in nutritional deficiencies. The bypassed portion of intestines was too severe.
As a result of these attempts, a wide array of combinatorial procedures were developed, including Duodenal Switch, Bilio Pancreatic Diversion, and Gastric Bypass.
These methods did not rely solely on malabsorption; they also utilized restrictive techniques, creating a smaller usable stomach. By incorporating both malabsorption and restriction, surgeons were able to bypass a smaller portion of the intestines. This reduced the risk of nutritional deficiencies from the bypass while the reduced stomach size physically limited the amount a patient could eat.
In 1967, the first Gastric Bypass surgery was performed by Ito and Mason at the University of Iowa. This approach was then modified over the years into its current form.
This surgery is known as Roux-En-Y Gastric Bypass (RYGP). There are two ways to perform this surgery: the open incision method and the laproscopic method, which uses 5 small incisions to reduce post-operative pain and speed recovery.
There are two ways to perform Roux-En-Y Gastric Bypass; open and laparoscopic. The laparoscopic technique significantly reduces post-operative pain and shortens the length of your hospital stay.
Today’s laparoscopic gastric bypass has been performed hundreds of thousands of times. Its outcomes have been studied, its risks and benefits evaluated, and it’s often covered by insurance.
It’s an excellent weight loss solution and should be seriously considered by anyone interested in bariatric surgery.
Why are some people a success while other struggle? Check out our Complete Guide To Bariatric Surgery.
Benefits
Gastric bypass has historically been the most popular bariatric procedure (Bariatric Surgery Data Management and Reporting Worldwide). Since 2011 gastric sleeve surgery has grown quickly in popularity and in 2015 is the most popular bariatric surgery option (largely the result of Lap Bands losing market share). However, this should not take away from the merits of gastric bypass surgery. It is still widely accepted as the ‘gold standard’ for bariatric surgery. Here’s why:
- You will lose weight. On average, you will lose 70% of your excess body weight in the first 18 months after surgery.
- This study shows 77.5% of excess weight loss after 18 months. (Journal Of Obesity, 2013)
- You will not be able to eat large meals (restricted pouch/stomach size).
- You will get sick from eating too much sugar and/or carbs (dumping syndrome).
- You will absorb less calories from food (bypassed intestines).
- You will improve and/or eliminate type 2 diabetes.
- Medication for high blood pressure and/or high cholesterol may be eliminated.
- Your hormones may adjust from significant weight loss, increasing testosterone and improving metabolism. (ASMBS)
- Long term weight loss success – most studies show that 90% of patients maintain at least 50% of excess weight loss after surgery.
Once you lose weight and reduce medications it becomes easier to exercise. If you are able to implement regular exercise along with a healthy diet, you may lose more than the average excess weight loss listed above.
Anecdotally, you will have more energy, more confidence, and feel better after gastric bypass surgery. These benefits are hard to measure but this study shows 95% of patients reported an improved quality of life 1 year after surgery.
Surgery Day
 You’ve made it to surgery! You’ve completed your psych evaluation, your nutrition consults, your physician supervised diet, and you’ve survived the pre-op diet.
You’ve made it to surgery! You’ve completed your psych evaluation, your nutrition consults, your physician supervised diet, and you’ve survived the pre-op diet.
The night before your surgery, you will need to stop eating. Try to relax, take a hot bath, and focus on the reasons why you chose to have surgery. Fear and second thoughts are completely normal.
On the day of surgery, do not eat or drink anything (including water or coffee) unless your surgeon or anesthesiologist specifically gives you permission. When you arrive at the hospital, you will be admitted and will have to fill out paperwork including consents. You’ll meet the pre-op nursing staff, your anesthesiologist and often your circulating nurse (the nurse that will be with you in the OR). If you have concerns don’t be afraid to ask questions.
You will then change into your hospital gown. You may also be asked to wear a pair of graduated compression stockings that are specially designed to prevent any blood clots from occurring. Most facilities will provide anti-anxiety medication. An IV will then be inserted into your arm so that antibiotics may be administered and intravenous fluids and medications have a direct path to your bloodstream. The IV will remain until you are discharged.
You will then enter the operating room, and sticky pads will be placed on your chest to monitor your heart rate. An oxygen mask will be placed on your face and then anesthesia will be administered through the IV. You’ll count back from 10 and wake up in recovery.
Recovery
After Surgery
You did it! The scary part is over. Now the hard work starts.
Recovery time will depend on the size of the incision made. If you had laparoscopic gastric bypass surgery performed, you will likely stay in the hospital for 2 to 3 days. If your surgery became an open procedure (bigger incision) recovery and your hospital stay may last longer.
The area of the incisions will be sore in the days following surgery. In the hospital this is easily managed with medication. Your surgeon will likely have you stand and walk the same day of your surgery. This helps remove any gas left over from the insufflation (air used to expand your abdomen and provide room to operate) used during your procedure. You will likely be asked to walk around the hospital floor at least 3 times daily after surgery.
Many hospitals now have patient-controlled analgesia (PCA). This is a mechanism that allows you to press a button and administer pain medication for yourself.
Your surgeon will visit with you a couple of times after surgery and before you are discharged. Make sure you have and understand the discharge instructions as well as any prescriptions and/or medications that you will need once home.
Returning Home
It’s good to be home. But it’s also a little scary. You’re on your own now.

Take Your Pain Medication
You will be sore and the soreness/pain may get worse before it gets better. The doctor has prescribed you pain medication. Don’t wait to pick it up from the pharmacy. Have a loved one get it for you or get it on your way home from the hospital. Take it as prescribed. Pain medications can cause constipation. Your discharge instructions should include guidelines for handling constipation during your first few weeks after surgery.
Your doctor will expect you to walk whenever possible but don’t overdo it. You’ll be very tired. Remember, you haven’t eaten anything in a few days and just had major surgery. So again, don’t overdo it in those first weeks but do walk around the house frequently.
Hydrate
Drink your water. Dehydration becomes a real risk after surgery. Food provides us with a fair amount of our daily water. Without food, you will need to pay close attention to your water intake to prevent dehydration. Fill up a large water bottle with all the water you’ll need for the day and start sipping. DO NOT use a straw to drink your water. It’s easy to drink too much too quickly and you risk swallowing air which puts undue pressure on your new stomach. Small sips, no straws, all day.
Sleep
You may have plans of immediately starting exercise, cleaning the house, organizing and helping out the family. You will need to sleep. You’ll be tired. You’ll have time to clean and organize and everything else but for those first few weeks, plan on resting.
If you have a recliner you may feel more comfortable sleeping in it. A slight incline can alleviate some of the pain in your abdomen and reduce the risk of heartburn. If you don’t have a recliner, have a few extra pillows at home.
Activity
Coughing is often encouraged to expand your lungs and bring up any fluids that may remain after surgery. But coughing hurts after surgery. Many doctors recommend using a cough pillow. Hold this tight to your stomach when you feel the need to cough. It will prevent large movements in your abdomen and reduce pain.
Always follow your discharge instructions. It is typically recommended to not lift anything weighing over 15 pounds for at least six or seven weeks. Keep walking. Increase your distance as your body allows it. Test out the stairs once you feel up to it but take it slow. If a certain activity is too difficult or causes pain, don’t force it.
Incisions
Do not soak in a bath. It is often recommended to wait until your first follow-up appointment before showering. It’s important that your incisions have time to heal and stay clean. A little redness around the incisions is normal. Drainage, pus, and foul smelling odors at the incision sites should be reported to your surgeon.
Follow-up Appointments
Your first follow-up appointment is about a week after your surgery; if you have skin staples they may be removed at this time. About a month later, you will return for your second follow-up, and about month after that, you will go back for your third. Most doctors will then want to see you four months later (which is a half a year after your surgery) and then sixth months after that, which would be a year after your surgery was completed. Remember that these are only approximate times for your follow up appointments. Different doctors may have different schedules, or your condition might require more visits.
Don’t skip your follow-up appointments. Don’t be afraid to share your struggles and concerns after surgery. Your surgeon can’t help you get back on track if you are not honest with him or her.
After your annual checkup, most doctors will want to see you once a year. You will receive prescription refills and have routine blood work performed at each of these annual visits. The blood work ensures you are not nutrient deficient.
Diet
Your bariatric program should have robust, easy to understand diet guidelines and you should be very familiar with them before surgery. Prepping your house with recommended food products and protein shakes is advised.

Pre-Op Liquid Diet
A week or two prior surgery your surgeon or dietitian will ask that you start a pre-op diet. The pre-op diet for gastric bypass typically looks like this:
- 5 to 7 liquid meal replacement shakes per day. High protein, low carb shakes are recommended.
- 64 to 96 ounces of water per day. Use the Bariatric Surgery App to track this.
- Some surgeons may allow a small portion of vegetables daily.
The goal of the pre-op diet is to shrink the size of your liver so it’s easier for your surgeon to access your stomach during surgery. The pre-op diet is tough but important. You will be hungry, dizzy, and moody for the first couple of days. By day three you should start to feel better as your body starts to burn fat instead of carbs as your primary energy source.
Post-Op Dietary Guidelines
A strict diet must now be followed for several reasons. Your stomach is now much smaller and recovering. Your intestines have been cut and re-routed. There are staples in both of these areas holding the tissue together. It’s important to not put any undue stress on this tissue while it’s healing. Large meals, fibrous food, carbonated beverages can lead to a staple line leak. Do not risk a serious complication. Follow your post-op diet!
There are four phases of the post-op diet:
- Clear Liquids
- Pureed Foods and Protein Shakes
- Soft Foods
- Solid Foods
Phase One: Liquids
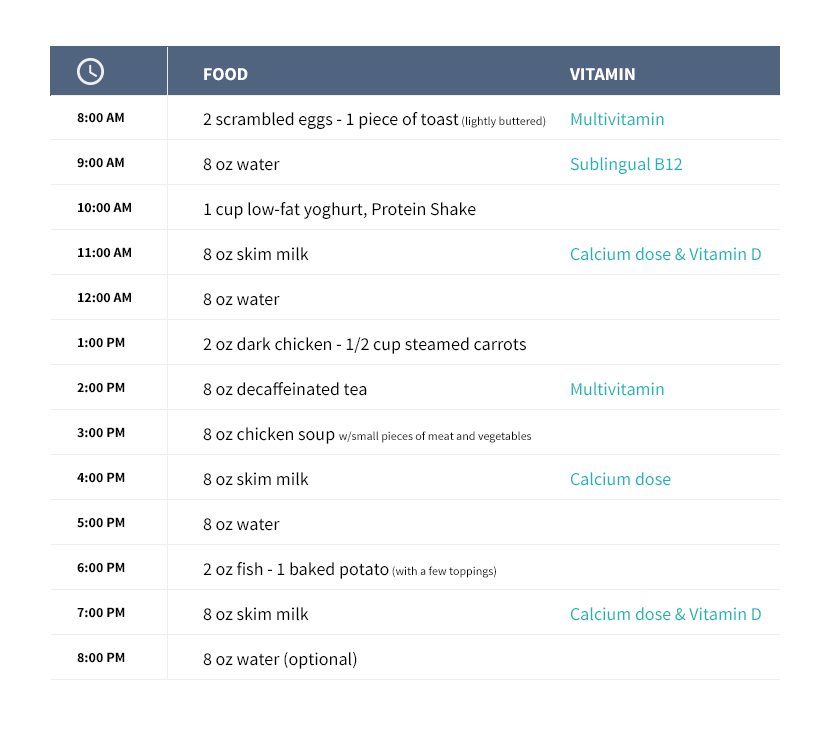
For about a week after surgery, only certain liquids are to be sipped slowly at the rate of two ounces per hour. Most dietitians and doctors will recommend items like water and sugar-free jello as well as fat-free broth and fat-free milk. The chart below shows a typical liquid diet for the first week after surgery.
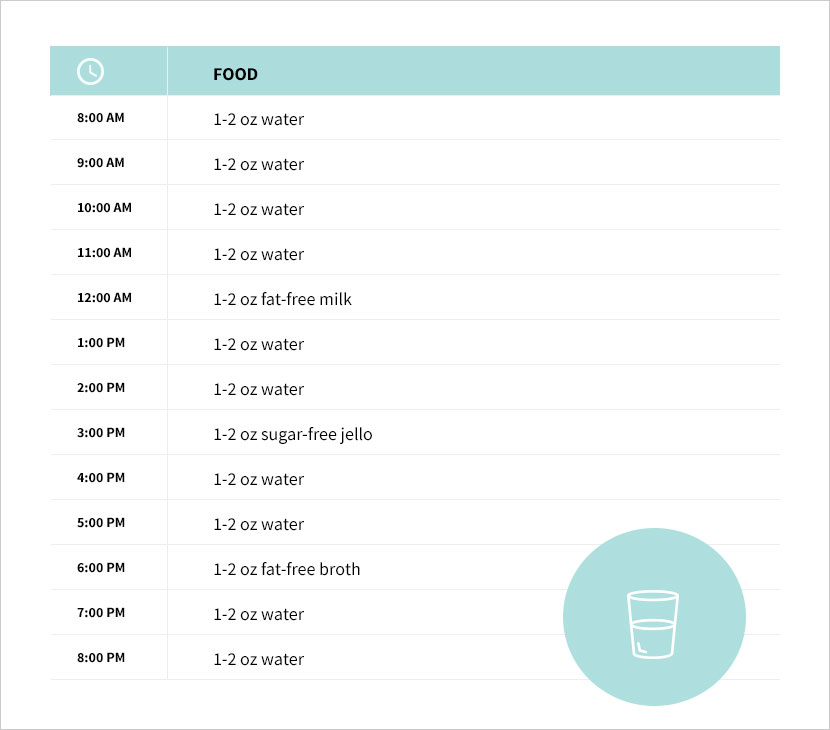
For more details on your phase one liquid diet, check out our Gastric Bypass Diet Guide.
Phase Two: Pureed Foods and Protein Shakes
Your doctor or dietitian will determine when the second phase will begin. For the next week or two, you will be able to consume pureed foods several times throughout the day in very small portions. During this phase, focus on eating slowly. Each small portion of soft food should be consumed over a 30 minute period. Eating each meal slowly, taking at least 30 minutes per meal, should remain a goal through all of the post-operative phases and beyond. The Baritastic app has a food timer that is handy for this purpose.
Most dietitians and doctors will recommend a daily intake of 60 to 70 grams of protein per day and about 64 ounces of the types of liquids consumed in phase one. Fat, sugar, caffeine, and carbonated beverages should be avoided. Your dietitian or doctor will probably allow you to consume egg whites, protein shakes, non-fat cottage cheese, and creamed soups with any chunks skimmed out. Wait at least 30 minutes before and after eating before drinking.
Below is a typical phase two diet schedule. Follow your doctors recommendations for vitamins and supplements. More phase two diet information can be found here.
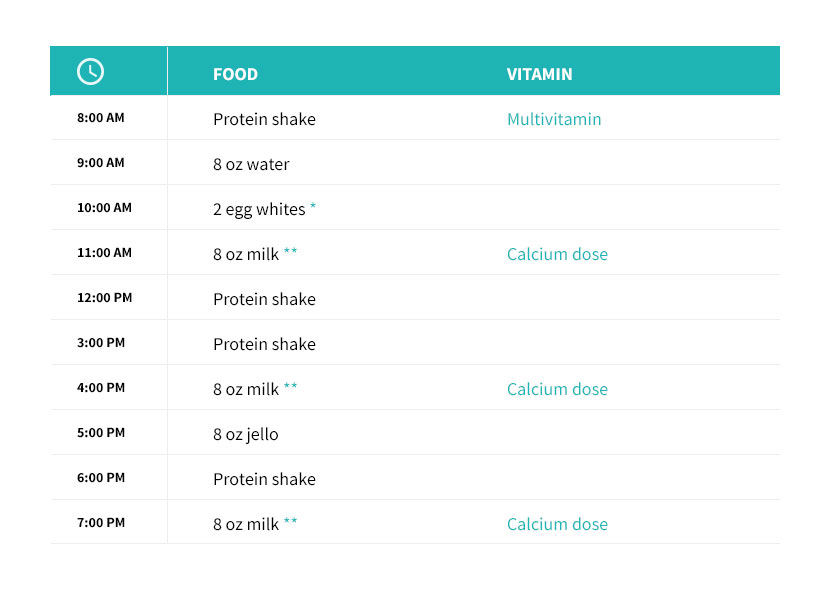
Phase Three: Soft Foods
During this part of your post-op diet plan, you will gradually begin to add food substances with more texture. This phase will usually last from one to three weeks, depending on the recommendations of your doctor or dietitian.
In this phase, you will be able to consume some lean meats and vegetables that are soft enough to be easily mashed with a fork, and your nutritional goals will remain the same as they were in phase two. A small amount of fat might be allowed.
Recommended soft foods will probably include items such as fish, egg whites, tofu, fat-free cottage cheese, fat-free cheese, canned tuna, and canned or shredded chicken softened with water. The vegetables that might be may suggested include avocados, mashed green beans, steamed carrots, and squash. Bananas will probably be allowed as well. However, bananas have a high sugar content. Break your banana into bite sized portions and only eat a bite or two in one sitting.
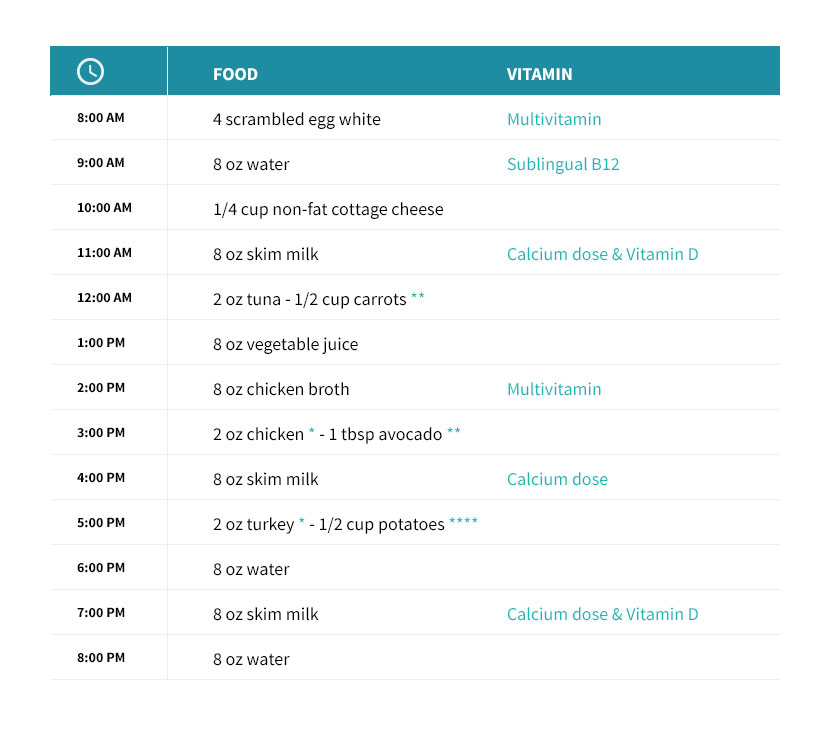
Phase Four: Solids
This is the last stage of your post-op diet plain. Go slow. Introducing new foods too quickly can cause painful gas, bloating, heartburn and dumping syndrome. Introduce one new food at a time. Wait a day before introducing another new food.
The goal in stage four is to re-introduce healthy foods in small portions. It is still recommended to start with softer foods and gradually work into chewy and fibrous foods.
Remember to take your time eating and continue to chew each bite of food well.
Keep track of your protein and ensure you are eating healthy vegetables as your primary carbohydrate source. Stay away from’ junk’ carbohydrates such as refined sugar, pasta, rice, bread, chips, etc.
You should now be able to reduce your meals per day to three small, nutrient dense meals (protein and vegetable). Supplement with your protein shakes and don’t forget needed vitamins and supplements.
Your total caloric intake will eventually reach 1,000 to 1,500 calories per day but do not force it. Certain foods are difficult for your body to process. Add them slowly and in small portions. These foods include corn, nuts, beans, beef, pork, shellfish, and grapes.
Check out our Gastric Bypass Diet Guide for more diet related information.
Dumping Syndrome – Good or Bad?
 Your body has a safety valve known as the pylorus. It prevents food from entering the small intestines until it has been broken down by gastric juices. The pylorus is bypassed during gastric bypass surgery. After gastric bypass surgery your stomach may prematurely dump its contents into the small intestines. This is called ‘dumping syndrome.’
Your body has a safety valve known as the pylorus. It prevents food from entering the small intestines until it has been broken down by gastric juices. The pylorus is bypassed during gastric bypass surgery. After gastric bypass surgery your stomach may prematurely dump its contents into the small intestines. This is called ‘dumping syndrome.’
Dumping syndrome causes abdominal discomfort, cramping, increased heart rate, diarrhea, dizziness, and nauseousness. It is very uncomfortable. Refined sugars are the primary cause of dumping syndrome but eating too much or too fast can also cause dumping syndrome.
Dumping syndrome is not good. And once you’ve experienced it, you will try to avoid it at all costs.
But dumping syndrome does reinforce your dietary guidelines. If you don’t eat small meals slowly, reduce or eliminate simple carbohydrates and refined sugars, you may experience dumping syndrome. This is a strong motivator to stay away from unhealthy foods.
Early dumping is a type of dumping syndrome that occurs less than half an hour after a meal, and its symptoms include sweating, nausea, cramps, diarrhea, dizziness, bloating, and vomiting. Late dumping is another form of dumping syndrome that occurs after an hour or more after a meal and includes most the symptoms of early dumping as well as hunger and fainting.
Vitamins & Supplements
After gastric bypass surgery your new stomach will restrict the amount of food you can eat. Your bypassed intestines will also reduce the amount of vitamins and minerals absorbed. It is necessary to take vitamins and supplements for the rest of your life after surgery.
It is important that you take the required vitamins and supplements after surgery for the rest of your life.
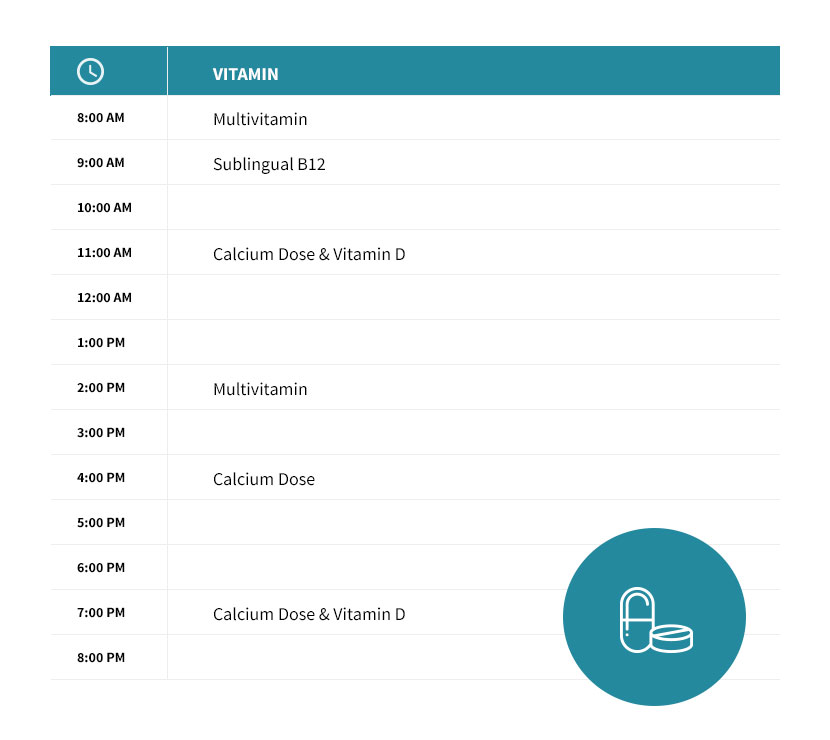
Multivitamin
You will need to take one or two multivitamins (depending on the type of vitamin) during the second or third phase of your dietary plan (always check with your surgeon). These multivitamins should be taken with meals, and this practice should continue for the rest of your life.
After surgery it can be difficult to swallow pills. You may want to consider vitamin patches. As always, check with your bariatric surgeon to ensure these vitamins meet your needs.
Calcium Citrate
Calcium citrate (usually somewhere around 500 mg three times/day) is an important nutritional supplement. It should be taken with meals but not at the same time as the multivitamin because the iron in the multivitamin will interfere with the absorption of the calcium. Some doctors and dietitians may want you to start calcium citrate in phase two and others may recommend you start it in phase three.
Note: Calcium citrate absorbs much better than calcium carbonate after gastric bypass surgery. Calcium carbonate is not recommended.
Vitamin D3
In either phase two or phase three, you will be required to begin supplementation with Vitamin D3. You will probably be instructed to take approximately 500 IU twice daily. These dosages should be taken with your calcium supplementation.
Vitamin B12
After your surgery, your digestive system will no longer be able to process adequate amounts of vitamin B12. 500 to 1,200 mcg of vitamin B12 in sublingual form is recommended. By taking it sublingually (under your tongue) it is directly absorbed into the bloodstream and does not have to enter the digestive tract where its bioavailability is reduced.
You also have the option of receiving monthly injections of B12. You can perform these injections yourself or have them administered by your doctor at your monthly checkups.
Iron
Iron is absorbed in the duodenum, which is the part of the small intestine that is bypassed after gastric bypass surgery. As a result, your body is no longer able to absorb adequate amounts of iron. The iron received in multivitamins may not be enough, and your doctor may want you to begin iron supplementation. This is particularly true for females during their monthly cycle.
Your doctor may also recommend that you also begin taking vitamin C because it helps your body better absorb iron. The amount and type of iron to be taken will also be determined by your doctor. Many patients are prescribed 500 to 1,000 mg of elemental iron per day. Ferrous fumarate and ferrous gluconate are the two most bioavailable forms of iron supplementation.
It is important to note that you do not want to take iron at the same time as calcium because they interfere with each other’s absorption.
Can it be Stretched?
 Yes. The stomach is made up of folds of tissue called rugae that expand and contract to accommodate food and liquid. The stretching of the stomach may be partly responsible for the feeling of ‘fullness’ after meals.
Yes. The stomach is made up of folds of tissue called rugae that expand and contract to accommodate food and liquid. The stretching of the stomach may be partly responsible for the feeling of ‘fullness’ after meals.
If you eat a large meal your stomach will stretch and then later contract. If you continue to large eat meals, you may start to feel like you ‘require’ a large meal to get ‘full.’ This can cause a cycle of eating to fullness, then eating before your stomach has fully contracted and feeling like you need more and more food to feel ‘full.’
Below are a few tips to help prevent stretching your stomach after gastric bypass.
- Do not eat until you feel ‘full.’ Eat a predetermined sized meal that is appropriate for how far out you are from surgery.
- If the amount of food on your plate is more than the size of your fist, you are probably eating too much.
- Don’t drink and eat at the same time. Both liquid and food end up in your stomach. Separate liquids and food by at least 30 minutes.
- Don’t drink carbonated beverages. The bubbles can put undue pressure on your stomach.
- Eat slowly and chew well.
For more information on stretching your stomach after gastric bypass, check out this article.
Expected Weight Loss
You can expect to lose between 60 to 80 percent of your excess weight from gastric bypass surgery. Most of the weight loss occurs in the first 18 months after surgery. There is a risk for weight regain after surgery, but gastric bypass surgery has one of the best long-term weight loss profiles when compared to other primary treatments for morbid obesity.
Gastric bypass is a tool to get your weight down to a healthy level. Once your weight is down it’s up to you to implement healthy habits that maintain or improve the weight loss. Below are a few healthy habits that will help sustain and/or improve your overall weight loss after surgery.
- Eat three small nutrient dense meals per day.
- Exercise 3 to 5 times per week.
- Journal what you eat. The Baritastic app is great for this.
- Follow-up with your surgeon as recommended. You’d be surprised at how many people don’t come back after 6 months.
- Attend support groups.
- Make friends, join forums.
- Get your family members to implement a healthy lifestyle.
If you’d like to calculate your expected weight loss after gastric bypass, you can use the calculator below. Note that this calculator is based on the average excess weight loss of 70% after gastric bypass surgery. You can lose more if you implement healthy habits.
The calculations are based on average weight loss per procedure. To lose the average amount of weight, you’ll need to follow your surgeon’s pre-operative and post-operative guidelines.
Long term diet and exercise changes along with other habit changes can lead to weight loss that exceeds the averages used in these calculations.
On average gastric bypass patients lose about 70% (Bariatric Surgery, A Systemic Review and Meta Analysis, 2004) of their excess weight. Gastric sleeve patients lose about 60% of their excess weight. And Lap Band patients lose about 50% of their excess weight.
Saggy Skin
Saggy or loose skin is common after losing lots of weight quickly. Regardless of the procedure or diet used to lose weight, if you are morbidly obese and lose weight quickly, you may have saggy skin. This is a reality.
 There are procedures to remove skin after gastric bypass surgery. Occasionally, these are covered by insurance.
There are procedures to remove skin after gastric bypass surgery. Occasionally, these are covered by insurance.
Over many years, your skin stretched as your body grew. While skin does have some elasticity, it will likely not fully tighten to match your new smaller body.
Age plays a role. Younger patients tend to have more elasticity in their skin. As we age our skin naturally loses elasticity. And younger patients have typically been overweight for a shorter amount of time. The skin is able to ‘bounce’ back quicker in these patients.
The total amount of weight lost plays a role. If you lose 200 to 300 pounds, you will likely have extra skin. If you lose 50 to 100 lbs, you will likely have less. And if you’re young, you may have very little if any loose skin.
This seems pretty obvious but it’s important. Setting proper expectations will help with your overall satisfaction and happiness after surgery. The goal of bariatric surgery is to improve your health by reducing the comorbidities associated with obesity. This is not a cosmetic procedure.
Below are a few things you can do that may help reduce (not eliminate) saggy skin after gastric bypass surgery. These are anecdotal.
- Hydrate. Drink plenty of fluids to keep your skin healthy.
- Moisturize.
- Exercise using weights.
- Stretch. Yoga or calisthenics can help build long lean muscles which can create a more ‘toned’ look.
- Eat fruits and vegetables.
- Use sunscreen daily. Sun can damage the skin and may reduce elasticity.
Emotional & Mindset Changes
Prepare for emotional changes after gastric bypass surgery. Imbalances of estrogen, progesterone and testosterone are related to depression (Holtorfmed). Losing weight changes your balance of testosterone, estrogen and thyroid production (Surgery for Obesity and Related Diseases, 2007).
This can be a welcome change as increased thyroid hormone can increase energy in patients with subclinical hypothyroidism. However, losing weight quickly after surgery may alter testosterone and estrogen levels. These hormonal changes can cause a range of difficult emotions. Depression, anger, feelings of hopelessness, and regret are not uncommon during the first year after surgery.
Expecting and preparing for these emotional changes can help reduce their impact. Attend support groups and prepare your family and friends. Over time, your hormones and emotions will find stability.
It’s also important to note that many patients have surgery and never experience emotional instability.
Jenna provides excellent insight into life after weight loss surgery: The Hardest Part of Weight Loss Surgery
Gastric Bypass Risks
While the benefits of gastric bypass are impressive, the risks need to be weighed carefully.
Below is a chart showing the most common complications and risks after gastric bypass surgery.
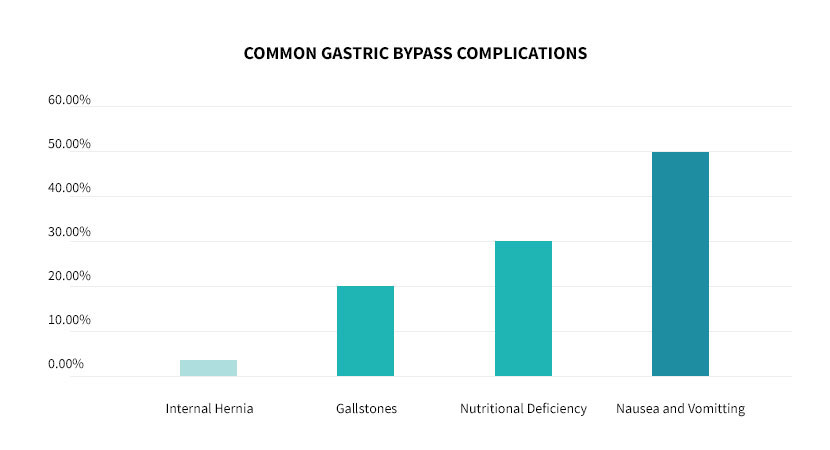
References: Canadian Journal of Surgery, Cleveland Clinic
Notes: Dumping syndrome is discussed here. Nausea and vomiting is not a true complication but common post-operatively and typically resolves with time and proper diet. Nutritional deficiencies are rare if the vitamin and supplement regimen is followed.
Major Complications
The chart above shows the common minor complications. The chart below shows the risk of serious complications after surgery.
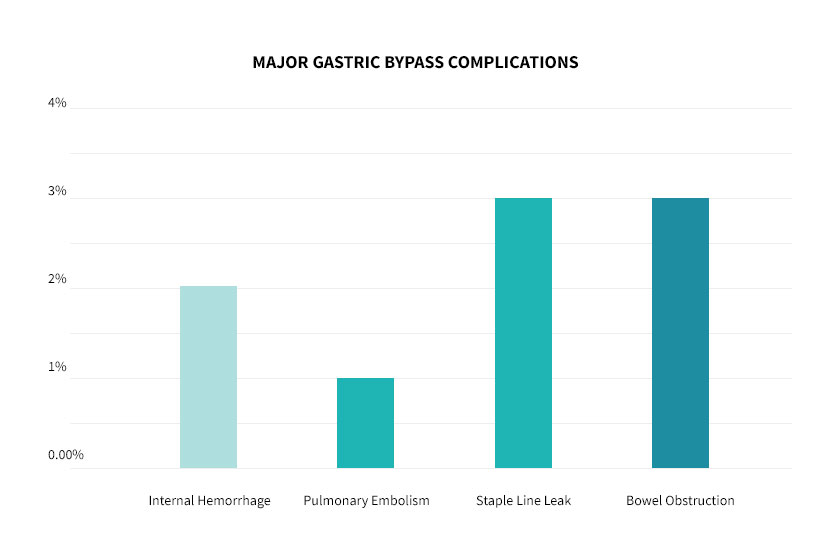
References: Schauer, CC, Annals of Surgery
Major complications can result in death. The risk of death after gastric bypass is less than 1% according to most studies. The mortality rate (death) from gastric bypass surgery is similar to the mortality associated with common surgical procedures such as gallbladder removal.
Pulmonary Embolism
This condition is caused when a blood clot forms after surgery and then travels to your lungs where it prevents proper blood/gas exchange. Its symptoms include chest pain, shortness of breath, shock, fainting, rapid heart rate, and death. Most instances of this condition can be treated with blood thinners (anticoagulants); however, if the condition is life threatening, thrombolytics (special medicines that are capable of breaking up large clots) or surgery may be required.
Staple Line Leaks
Leaks usually happen when the tissue holding the staples disintegrates or when the staples themselves fail. This creates a hole where the contents of your bowel and/or stomach leak into your abdomen. These leaks can often be repaired if they are discovered early enough. Symptoms include severe pain, increased heart rate, and fever.
There are two primary ways that surgeons will check for leaks; a pouch test using air while looking for bubbles or injecting dye and then looking for the dye in the abdomen. Minor leaks are typically treated by resting the stomach and feeding the patient with an IV; however, sometimes surgery is required for more severe leaks.
Small Bowel Obstruction
Small bowel obstructions may occur shortly after surgery or years later. Symptoms include abdominal pain and swelling as well as vomiting. A diagnosis can be made with either a CAT scan or surgery. Treatment of this condition might require surgery.
Other Risks and Downsides
Pregnancy
Women of childbearing age should wait 18 months after surgery before getting pregnant.
Nausea
Nausea is a normal occurrence for many people who have had gastric bypass surgery. And your chances of experiencing this condition are about 70 percent. Usually, nausea is caused by noncompliance with the dietary guidelines given to you by your doctor. Remembering to eat the correct things, not drinking while eating, and chewing your food properly will reduce nausea.
Dehydration
This condition occurs when your fluids have been depleted. The best way to prevent dehydration is to sip plenty of fluids throughout the day. This is particularly important the first week after surgery when you can only take small sips. Fill up a bottle with 64 ounces of water and slowly sip every few minutes.
Indigestion
Indigestion is usually accompanied by discomfort in the upper portion of your abdomen. This condition is treated by drinking only fluids for a certain period of time and completely avoiding greasy foods. If changes in your diet fail to alleviate this condition, antacids may be used as form of treatment. But, as always, consult your doctor before self-medicating.
Wound Site Infection
Wound site infections have a wide range of incidence (from 1.5% to 20%) and it may be related to the technique used to create the gastro-jejunostomy (stomach to intestine anastamosis). If treated early, wound site infections can be managed with antibiotics. Open procedures have a higher risk of wound site infections.
Ulcers
After gastric bypass surgery there is a risk of ulcers. Smokers and people who use certain medications are at a higher risk of developing post-operative ulcers. Below is a list of common medications to avoid after surgery. This list is not comprehensive. Your discharge instructions should include a complete list of medications to avoid. And do not smoke. Smoking increases your risk of ulcers.
- Alka-seltzer
- Ibuprofen
- Excedrin
- Motrin
- Pepto-bismol
Other Complications
There are other complications that are not discussed in this article. They range in severity and include strictures, tissue ischemia, internal hernias, and gastric reflux (heartburn) among others.
What Does It All Mean?
Gastric bypass is considered a safe procedure. The average complication rate is 5.9% in the first 30 days after laparoscopic gastric bypass surgery (MBSQAIP). And the risk of death is similar to the risk of death with common surgical procedures such as gallbladder removal.
Books & Tools For Success
There are many books about gastric bypass surgery. If you’re like me and enjoy reading before bed, the books below are excellent.
The Emotional First Aid Kit: A Practical Guide to Life After Bariatric Surgery, Second Edition
This book is a must read for anyone considering gastric bypass surgery. The real work starts one or two years after surgery. This book examines your emotional mindset, prepares you for the unexpected, and puts you on the path to long-term success.
Weight Loss Surgery For Dummies
This is a nice-to-have reference guide for anyone considering weight loss surgery. It’s not specific to gastric bypass but it is comprehensive. It’s well written and the perfect book to leave on your nightstand and reference when needed.
Eating Well After Weight Loss Surgery
While the Baritastic app has a number of recipes, this book is a handy guide to keep in your kitchen. The recipes are both delicious and nutrient dense. This book has meal plans tailored to gastric bypass patients. The meals are low carb, high protein using real unprocessed ingredients. Think your limited to chicken and eggs after surgery? This book offers a ton of creative recipes.
Baritastic iPhone and Android App
The Baritastic app is a must-have tool for anyone that has had or is considering weight loss surgery and it’s totally free. The app has some great recipes, a food/water timer, a journal, a newbie checklist to help you get to surgery and a social support aspect as well. It has a full nutrition tracker and needed resources for anyone that has had weight loss surgery.
Conclusion
Gastric bypass surgery is a well studied effective treatment for morbid obesity. While there are new surgical procedures for weight loss, none have the long-term data, excellent results and safety profile that gastric bypass has repeatedly shown. Gastric bypass remains the ‘Gold Standard’ for weight loss surgery and should be strongly considered by all bariatric surgery candidates.

